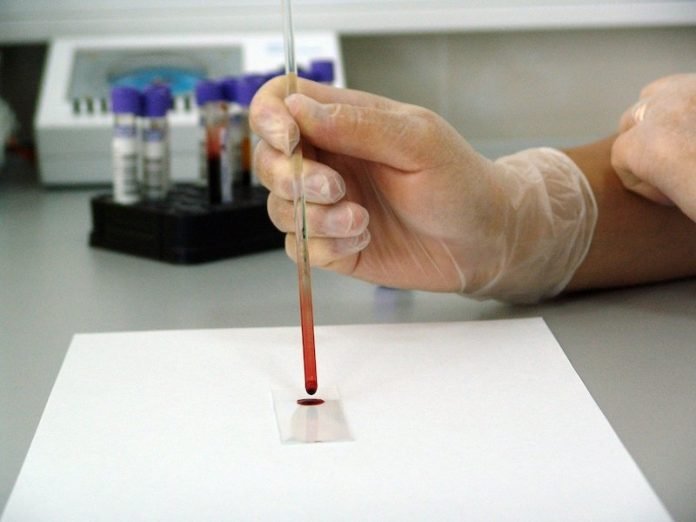
In three new studies, researchers provide convincing evidence that an in-house developed blood test for Alzheimer’s disease can detect the disease early and track its course.
The finding has major implications for potential use in clinical practice and treatment trials.
The research was conducted by a team from the University of Gothenburg.
After decades of research, scientists now know that Alzheimer’s disease-related memory problems are just the tip of the iceberg of underlying degenerative processes in the brain that have been silently developing over years or even decades.
These processes result from the abnormal aggregation of amyloid and tau proteins in the brain, with these aggregates being the defining pathological features of Alzheimer’s disease.
Until recently, it was only possible to detect these protein aggregates in the brains of deceased patients at autopsy.
Recent research advances, however, have enabled the accurate detection of amyloid and tau pathology in the brain with imaging methods and in the cerebrospinal fluid of living individuals.
These current so-called biomarker methods are either expensive, invasive, or only available at specialized centers; thus, only a fraction of patients suffering from the disease currently benefit from these advances.
An accessible, affordable, and minimally invasive biomarker for Alzheimer’s disease would revolutionize the care of patients worldwide, as well as boost the development of novel drugs for this presently still incurable disease.
Previously, the team had discovered such a biomarker: a cheap blood test capable to detect the presence of phosphorylated tau protein (p-tau181), a principal, defining hallmark of Alzheimer’s disease.
In the new studies, the team demonstrated great potential for the blood test to predict and monitor Alzheimer’s disease progression in an unprecedently large study comprising more than 1100 subjects, followed up over several years.
They analyzed participants’ blood samples acquired at different ages to construct the temporal trajectory of p-tau181 levels in blood across the long course of Alzheimer’s disease.
Importantly, they found that the novel blood test could detect abnormalities in p-tau181 levels several years before the onset of memory loss, suggesting enormous potential for early disease detection.
They also demonstrated the high clinical utility of p-tau181 in blood for predicting future Alzheimer’s disease dementia, even among individuals who had not experienced any memory impairment at the moment of the blood test.
Finally, they showed that annual increases of p-tau181 in blood were strongly coupled to the loss of nerve cells in Alzheimer’s disease as well as to cognitive decline.
Together, these studies represent a crucial step towards the widespread use of biomarkers in clinical routine, making effective blood biomarker testing for Alzheimer’s disease a reality for most clinical settings, including primary care.
One author of the study is Michael Schöll, an associate professor.
The study findings are published in Molecular Psychiatry, Brain, and JAMA Neurology.
Copyright © 2021 Knowridge Science Report. All rights reserved.



