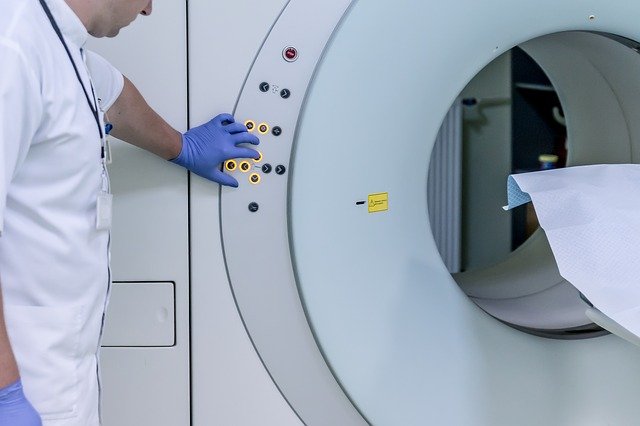
There are two types of lung cancer: non-small cell lung cancer and small cell lung cancer.
Smoking tobacco can cause most lung cancers, but sometimes nonsmokers can also develop lung cancer.
Lung cancer screening has been found to reduce deaths from the disease, but does that mean everyone should do it?
In a recent article, experts from Michigan Medicine explain this.
In the lung cancer screening, a person has a CT scan. If there is a spot on one of the lungs, whether it is cancer can only be determined by a biopsy.
But biopsy is not risk-free. During the procedure, there can be complications. For example, one of the lungs collapses. The patient recovers, and it turns out the spot isn’t cancer.
Now another patient has the same lung cancer screening and has a spot on the lung. This time it is lung cancer.
But in fact, the second patient is the exception to the rule; most spots or “nodules” are not cancerous.
The stories the second patient’s that make headlines, and people may believe that lives can be “Saved by the Scan.”
They ignore the complexity of screening.
So who needs lung cancer screening?
According to The U.S. Preventive Services Task Force, people ages 55 to 80 who have smoked at least 30 “pack years” (the equivalent of a pack a day for 30 years) and are either current smokers or have quit within the past 15 years should do lung cancer screening.
There is research evidence showing that in a similar group that CT screening, compared to chest X-rays, lowered the risk of dying from lung cancer.
About 154,000 Americans are expected to die of lung cancer this year. That’s more than cancers of the colon, breast and prostate combined. Lung cancer is by far the leading cancer killer.
Even if it hasn’t endured smoking, the lung is an organ that wears its scars like ribbons earned in battle.
Even coughs or colds affect what you see on a computed tomography or CT scan. So if you plan to allow something as invasive as a biopsy, you should know the implications.
Many doctors may not know who would benefit most from lung cancer screening. They often overestimate the benefits and underestimate the risks of screening.
For example, a patient from a few years ago who was screened for lung cancer and then came in for a $6,000 PET scan to look for lung cancer.
The patient entered the office in a wheelchair, on oxygen, weighing around 350 pounds and unable to walk across the room.
Given all these complicating factors, it is reasonable to say this patient should not be screened.
So what is the disadvantage of lung cancer screening?
Screening itself is a misunderstood concept, one that goes beyond a single test. Many screenings can be burdensome.
A freckle can be harmless, but nonetheless requires months of follow-up.
In the lungs, most abnormalities found by a CT scan are “more often the result of old infections, scar tissue or other causes,” according to the ACS.
But this gets lost in the marketing messages promoting screening.
You don’t hear about the patient whose lung collapses during a biopsy, or the one with other complications during an invasive procedure, or those panicked with worry waiting for a diagnosis that may never come.
Now researchers are working to create something that could help people learn about screening, its pros and cons, and help them measure their cancer risk.
New guidelines and recommendations to interpret the results of screening have been put in place to minimize the rates of false positives and improve the value of screening.
So hopefully screening in practice will work even better than the way it did in the clinical trials.
Copyright © 2018 Knowridge Science Report. All rights reserved.



