Katy Connors, 40, was born with a rare heart disease. She had regular checkups with cardiologists most of her life, and knew she’d need a valve replacement at some point.
The condition, known as unicuspid aortic valve, hadn’t caused many issues in her life, not even through her six pregnancies.
On Sept. 1, 2022, Katy Connors was pregnant for the seventh time and about eight weeks along when she saw Michael Joynt, M.D., a cardiologist who specializes in caring for children and adults with congenital heart conditions at the University of Michigan Health C.S. Mott Children’s Hospital Congenital Heart Center.
At that appointment, Katy Connors and her husband, Brad Connors, were shocked to learn that her valve was almost completely narrowed.
She was in heart failure.
“With all my other pregnancies, I never had any issues. So, when I came in for this appointment, I was completely blown away,” she said. “Looking back, I was symptomatic, but I just didn’t recognize the signs.”
On a trip to Mackinac Island, for example though, she had struggled to climb stairs to a lookout point.
“I couldn’t breathe. I just thought I was out of shape but, looking back now, it’s because my valve was so closed it was really hard to breathe,” she said.
Joynt said when physicians decide how risky a pregnancy is for a patient, they’re given a rating of I through IV, with IV the riskiest.
“Katy’s aortic lesion is a class IV. She had one of the highest-risk heart conditions you can have while pregnant,” Joynt said.
Joynt began seeing her every couple of weeks as an outpatient, along with Elizabeth Langen, M.D., a maternal-fetal medicine specialist and the maternal-fetal medicine director of the cardio-obstetrics program at U-M Health Von Voigtlander Women’s Hospital.
“We talked to her about the risks involved in continuing a pregnancy with the condition that she had,” Langen said.
“She heard and understood those risks and wanted to continue and have a safe outcome for her and her baby.”
Hospitalized in “the Hallmark room”
At 13 weeks pregnant, her condition couldn’t be managed at home anymore and she had to be hospitalized.
“I was starting to show a lot of symptoms—when I laid down I couldn’t breathe, I was swelling up all over. With all my other pregnancies, I had preeclampsia and my symptoms were mimicking preeclampsia, but at 13 weeks that shouldn’t happen,” Connors said.
“My heart needed me on IV medicines and, being pregnant, they wanted to make sure I was being continuously watched because if something were to go wrong, it could be an emergency situation.”
With six children at home, Connors’ long-term hospitalization challenged the family.
She missed Thanksgiving, Christmas and her 40th birthday at home. But her U-M Health care team did everything they could to make the family feel welcome.
“They called my room ‘the Hallmark room’ because it was decorated for the holidays,” she joked.
Her kids—Jack, 15; Josie, 13; Charley, 12; Lillie, 10; Henry, 9, and George, 7—even brought in their Christmas presents from Santa Claus so they could open gifts with her.
“It’s been really cool to be in such a family-centric hospital that’s been really welcoming to my children,” Connors said.
From the care team’s perspective, they focused on keeping her well enough to continue the pregnancy.
“We were hopeful we wouldn’t have to do it, but we considered a high-risk aortic valve intervention just to be able to get her to the point of viability,” Joynt said.
“That’s about 23 weeks for a baby to even have a chance to survive.”
Joynt had weekly meetings with the adult cardiac interventional team, including Devraj Sukul, M.D., to discuss her status and how physicians would need to potentially emergently intervene.
Delivering Teddy
At 26 weeks gestation, her breathing issues became so severe, it was time to deliver the baby.
“Sometimes our patients who have heart disease will recover and get a lot better when the stress of pregnancy is taken away,” Langen said.
“Katy had a major valve issue—we knew she would need surgery; we just didn’t know how soon after delivery that would be.”
In a massive care coordination effort, Langen performed a cesarean delivery with Connors under general anesthesia by specialized cardiac anesthesiologists (led by Amanpreet Kalsi, MBBS) in a cardiac operating room at Mott with a cardiac surgery team present.
The cardiac surgeons were ready to intervene just in case her heart fared too poorly during delivery.
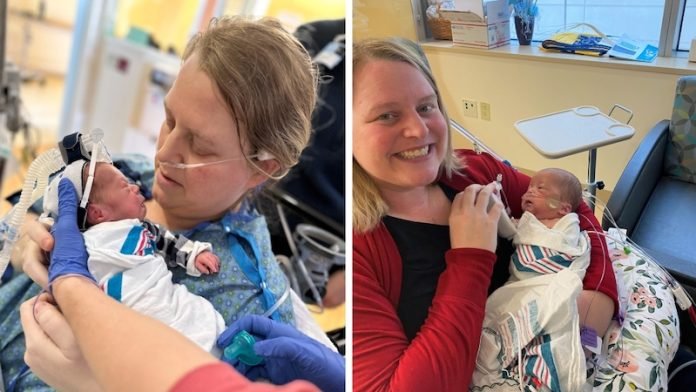
But all went as well as possible given the circumstances, and baby Teddy arrived January 27 at 2 lbs., 1.12 oz. He entered the Newborn Intensive Care Unit at Mott.
From there, the teams monitored both mother and baby.
“For better or worse, we have the honor of taking care of a lot of very sick moms during their pregnancy. It happens periodically that we have a mom admitted to one ICU and her baby admitted to the NICU,” said Langen.
“We try to help mom and baby connect as much as possible. If one or the other is more stable, we try to coordinate visits to the other in their respective ICUs, or otherwise, help mom and baby connect with pictures, videos—anything we can do.”
After Teddy’s birth, Connors remained hospitalized for two weeks. She then stayed at a Ronald McDonald facility for three weeks to be near Teddy and reduce her own risk of infection while she recovered from the c-section and prepared for open-heart surgery.
Open-heart surgery
To fix the valve issue, Connors opted for a Ross procedure with Vikram Sood, M.D., and Tim Lancaster, M.D., congenital and pediatric acquired heart disease surgeons at Mott.
The Ross procedure is a complex operation in which a patient’s native pulmonary valve is moved into the aortic valve position, and a secondary pulmonary valve is attached in place of the initial native pulmonary valve.
Because the procedure involves two valves, rather than one like a mechanical or bioprosthetic aortic valve replacement, it can be considered a riskier operation.
But Sood, Lancaster and Joynt believed the benefits outweighed the risks in Connors’ case.
The Ross procedure is frequently used in children who need an aortic valve replacement because the patient’s native pulmonary valve can grow along with the child (and there are not small enough aortic valve replacements for small children on the market).
A Ross procedure appealed to Connors over a more conventional, mechanical valve replacement because a mechanical aortic valve requires anticoagulation medication for life, and adds significant risk to future pregnancies, something Connors wasn’t willing to do.
Because Teddy’s delivery went well, the cardiac surgery team wanted to wait as long as possible to operate, allowing Connors time to recover from one surgery and cope with life as a mom with a child in the NICU.
At about six weeks postpartum, her cardiac team determined her heart couldn’t wait any longer.
Sood and Lancaster operated on March 9 and the surgery was a success. Conners’ postoperative course was uncomplicated, and her echocardiogram demonstrated a well-functioning, new aortic valve.
“All things considered, she’s doing great. She was really sick from her aortic valve stenosis, but she safely delivered a child and was well enough to take on a major open-heart procedure for herself,” said Sood.
“We don’t operate on someone who is six weeks postpartum on a daily basis, but cases like this showcase the hospital’s particularly unique style of having multiple teams work together in a really seamless way. This is what we do,” he added.
A “remarkable” mother
A few weeks post-operation, Connors went home after 188 long days in the hospital. Her family is thrilled to have her home while they continue to support Teddy in the NICU.
His original due date was April 30, and they’re hoping he can come home soon.
Joynt says that between Connors’ care from the adult cardiac team, who treat some of the hospital’s oldest patients, and Teddy’s care in the NICU, their case spanned an astonishing spectrum.
“Katy’s positive attitude and the great collaborative care is really what provided such an outstanding outcome for her,” Joynt said.
Connors said, “We still don’t know with Teddy what tomorrow will bring, but we are hopeful and very grateful that everything has gone as well as it has gone.”
She adds that the family’s prayer life has helped them tremendously. She’s also treasured the love her older kids show for their tiny baby brother.
“The thing that amazed me the most was the people praying for me, Teddy, and our family—literally from all around the world, kids from schools across the country sent cards to let us know they’re praying for us,” she said.
Joynt says he saw this firsthand, and that many people at the hospital felt connected to Connors and her saga.
“Her story is something so many people can relate to. Whether you’re a woman who has gone through pregnancy, or a spouse, so many people can put themselves in her shoes and think ‘I can’t believe all you’re doing [for your baby]’,” Joynt said.
“She did such a great job throughout everything, and we all wanted nothing but the best for her.”
Langen says her case illustrates the resilience of moms she works with every day.
“Katy just exemplifies the strength and grace that a lot of our moms have, especially those dealing with heart disease,” Langen said.
“Heart disease would incapacitate a lot of people, and these women are caring for a newborn child at the same time.
It’s remarkable what she was willing and able to do to have a successful pregnancy, and she’s just one of so many amazing examples.
Written by Annie Clarkson.
If you care about heart health, please read studies about the best time to take vitamins to prevent heart disease, and flu and COVID vaccines may increase heart disease risk.
For more information about health, please see recent studies about how drinking milk affects risks of heart disease and cancer, and results showing strawberries could help prevent Alzheimer’s disease.



