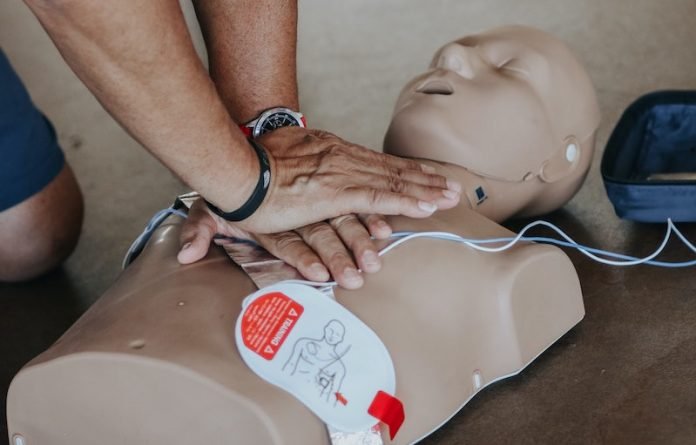
Sudden cardiac arrest (SCA) is when the heart suddenly stops working, usually because of a problem with its electrical system.
This can happen to anyone and may cause a person to suddenly lose consciousness, stop breathing, and have no pulse.
It’s different from a heart attack, which happens when the blood flow to the heart is blocked.
SCA is a medical emergency and needs quick treatment, like CPR and defibrillation, to help the heart start beating normally again.
Some things that can increase the risk of SCA are heart disease, high blood pressure, smoking, and not getting enough exercise.
Treatment for SCA can include medication and lifestyle changes like eating healthy and exercising.
What Did the Study Find?
In a new study, University of Utah Health scientists have found a potential new strategy for treating abnormal heart rhythms caused by a genetic condition called arrhythmogenic cardiomyopathy.
The condition is one of the leading causes of sudden cardiac arrest in athletes under the age of 35.
Scientists have found that restoring healthy levels of a protein called GJA1-20k, which heart cells need to establish connections with one another, corrected abnormal heart rhythms in mice.
This protein is underproduced in people with arrhythmogenic cardiomyopathy.
The findings have significant implications for the treatment of arrhythmias caused by arrhythmogenic cardiomyopathy and may also be relevant for treating dangerous arrhythmias that can occur soon after a heart attack.
Arrhythmogenic cardiomyopathy is a genetic condition in which people are born with normal hearts but develop an irregular heartbeat in their 20s or 30s.
These arrhythmias can raise the heart rate to dangerous levels, which is why some individuals with the condition experience sudden cardiac arrest during exercise.
Currently, patients diagnosed with arrhythmogenic cardiomyopathy are advised to restrict exercise and may benefit from an implantable defibrillator to control their heartbeat.
As the disease progresses, the heart muscle becomes fatty and fibrotic, preventing the heart from pumping blood efficiently, and eventually leading to the need for a heart transplant.
The scientists studied heart tissue from patients with arrhythmogenic cardiomyopathy who had undergone transplantation and discovered a problem with a protein called Connexin 43.
In healthy hearts, Connexin 43 forms channels between adjacent cells, facilitating communication.
The diseased hearts made normal amounts of Connexin 43, but it was not located where it belonged.
The team suggests that this was likely because there wasn’t enough of a trafficking protein, called GJA1-20k.
Previous studies had shown that without this protein, heart cells would not be able to get Connexin 43 to the right place.
To determine whether restoring healthy levels of GJA1-20k could restore the heart’s normal rhythm, the scientists used mice that have similarities to people with arrhythmogenic cardiomyopathy.
These mice have low levels of GJA1-20k and develop arrhythmias.
The researchers used low doses of gene therapy to bring the trafficking protein GJA1-20k back to normal levels.
This enabled heart muscle cells to transport Connexin 43 to its proper locations and restored a more normal heartbeat in the mice.
The treatment success in mice suggests that raising levels of GJA1-20k might restore normal heart rhythms in patients with arrhythmogenic cardiomyopathy.
The team says the ease and low dose needed to fix the arrhythmias of even an inherited heart disease suggests that we have identified a critical pathway to stabilize cardiac electrical activity.
The treatment success in mice suggests that this protein-based approach could potentially be a new paradigm for treating heart rhythm disorders.
Further research will be needed to develop the treatment for clinical use.
If you care about heart health, please read studies about best time to take vitamins to prevent heart disease, and Vitamin K2 could help reduce heart disease risk.
For more information about heart health, please see recent studies that calcium supplements may harm your heart health, and results showing COVID-19 vaccines may increase heart disease risk.
The study was conducted by Joseph Palatinus et al and published in the journal Circulation Research.
Copyright © 2023 Knowridge Science Report. All rights reserved.



