About one-fourth of people with diabetes develop painful foot ulcers, which are slow to heal due to low oxygen in the wound from impaired blood vessels and increased inflammation.
These wounds can become chronic, leading to poor quality of life and potential amputation.
Jianjun Guan, a professor of mechanical engineering & materials science in the McKelvey School of Engineering at Washington University in St. Louis, has developed a hydrogel that delivers oxygen to a wound, which decreases inflammation, helps remodel tissue and accelerates healing.
Results of the work, which were in a mouse model, are published in Science Advances.
Ya Guan, a doctoral student, and Hong Niu, a postdoctoral research associate, both in Guan’s lab, are co-first authors.
“The oxygen has two roles: one, to improve skin cell survival under the low-oxygen condition of the diabetic wound; and two, oxygen can stimulate the skin cells to produce growth factors necessary for wound repair,” Guan said.
Tissues in the body require oxygen to survive and need even more when tissue is injured.
While there are several existing treatments for chronic wounds in people with diabetes, the most common treatment is dozens of sessions in a hyperbaric oxygen chamber, but its effectiveness is inconsistent and includes the risk of oxygen toxicity.
Guan’s hydrogel delivers oxygen to the wound using microspheres that gradually release oxygen to interact with the cells through an enzyme on their surface that converts what is inside of the microsphere into oxygen.
The oxygen is delivered to the wound over about a two-week period, and inflammation and swelling decrease, prompting healing.
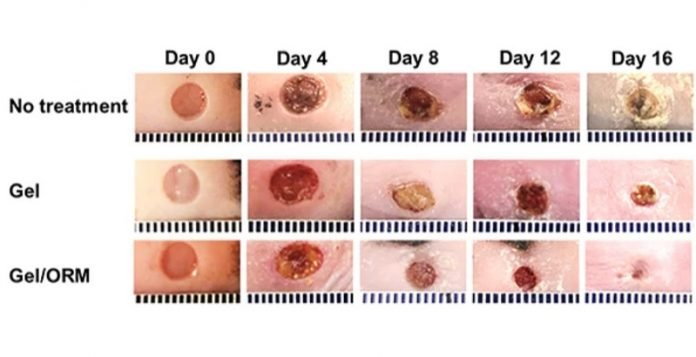
In the mice, wounds treated with the hydrogel containing the oxygen-releasing microspheres had a greater rate of closure than wounds treated with only the gel or those with no treatment.
By day 16, the wounds treated with the hydrogel had reduced to 10.7%. Those treated with the gel only were reduced to 30.4%, and those with no treatment had reduced to 52.2%.
In addition, the wounds treated with the hydrogel containing the oxygen-releasing microspheres had the thickest epidermis on day 8, but the thinnest by day 16, indicating the wound was healing and inflammation was reduced.
Over the past 14 years, Guan has been developing this type of gel, which has nearly 70 different functions and chemical structures.
“The gel is a liquid before we put it into the skin tissue, so it is easy to mix in the microspheres,” he said. “Once we put the mixture of the gel and the microspheres into the wound, it becomes a solid because it is temperature-sensitive — at lower temperatures it is a liquid, and at body temperature it’s a solid.”
One risk of delivering oxygen to wounds is delivering too much, which creates reactive oxygen species (ROS), which can damage or kill cells at elevated levels. Guan’s hydrogel is able to scavenge for ROS content and destroy it, eliminating any risk.
Next, Guan’s team plans to use the hydrogel in a large animal model with the expectation of future human clinical trials.
“This represents a new therapeutic approach to accelerating healing of chronic diabetic wounds without drugs,” Guan said. “It also has the potential to treat other diseases in which oxygen is low, such as peripheral artery disease and coronary heart disease.”
Written by Beth Miller.



