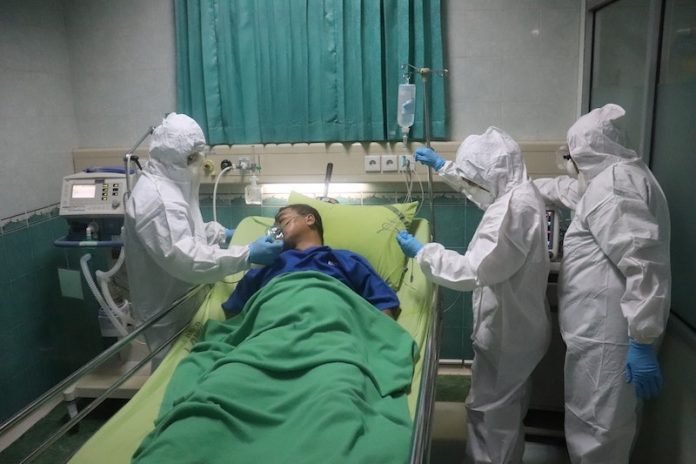
In a new study, researchers found that severe acute complications are common among adults hospitalized with COVID-19, leading to an inpatient mortality rate of 20%.
The research was conducted by a team from Premier Applied Sciences in Charlotte, North Carolina.
In the study, the team used a hospital administrative database to assess factors linked to in-hospital mortality among patients treated for COVID-19.
They identified 64,781 patients with COVID-19, with in-hospital mortality of 20.3%.
Among inpatients, 15.9% received invasive mechanical ventilation and 19.4% were admitted to the intensive care unit (ICU).
The average inpatient length of stay was six days, while the median ICU length of stay was five days.
Acute inpatient complications included acute respiratory failure (55.8%), acute kidney failure (33.9%), and sepsis (33.7%).
The risk factor most strongly associated with death was older age (age ≥80 years versus 18 to 34 years).
Decreased risk of death was linked to the use of statins, angiotensin-converting enzyme inhibitors, and calcium channel blockers.
Patients treated with a drug combination of azithromycin and hydroxychloroquine had an increased risk of death compared with patients receiving neither medication.
This study is the first to examine the treatment patterns and risk factors linked to COVID-19 mortality using a large national sample of patients with confirmed COVID-19 across all regions in the United States.
One author of the study is Ning Rosenthal, M.D., M.P.H.
The study is published in JAMA Network Open.
Copyright © 2020 Knowridge Science Report. All rights reserved.



