Responding to the COVID-19 pandemic caused by the novel coronavirus, SARS-CoV-2, requires models that can duplicate disease development in humans, identify potential targets, and enable drug testing.
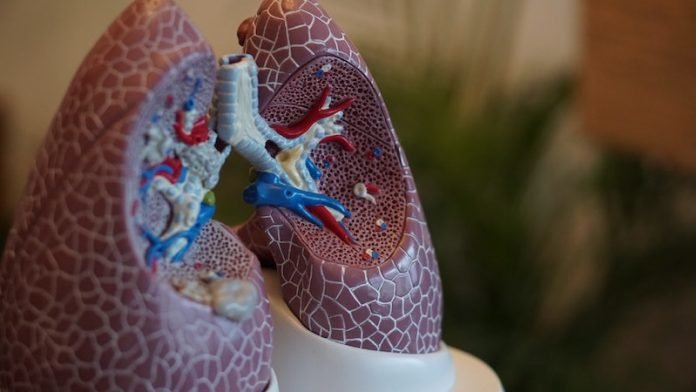
Specifically, access to the primary human lung in vitro model systems is a priority since a variety of respiratory epithelial cells are the targets of viral entry.
In a new study, researchers tested human stem cell-derived lung cells infected with SARS-CoV-2.
They found that the virus initially suppresses the lung cells’ ability to call in the help of the immune system with interferons to fight off the viral invaders and instead activates an inflammatory pathway.
The infected lung cells pour out inflammatory proteins. In the body of an infected person, those proteins drive up levels of inflammation in the lungs.
The research was conducted by a team at Boston University.
According to the team, the inflammatory signals initiated by the infected pneumocytes attract an army of immune cells into lung tissue laden with infected and already dead and dying cells.
The data confirms that COVID-19 blocks cells from activating one of the anti-viral branches of the immune system early on after infection has set in.
The signal the cells would typically send out, a tiny protein called interferon that they exude under threat of disease, are instead delayed for several days, giving COVID-19 plenty of time to spread and kill cells, triggering a buildup of dead cell debris and other inflammation.
The data is based on experiments the research team performed in the laboratory.
They developed sophisticated models of human lung tissue, which has been used to study a range of chronic and acute lung diseases.
The team says these cells are an amazing platform to study SARS-CoV-2 infection. They likely reflect what is going on in the lung cells of COVID-19 patients.
One author of the study is Darrell Kotton, MD.
The study is published in Cell Stem Cell.
Copyright © 2020 Knowridge Science Report. All rights reserved.