In a new study, researchers at Johns Hopkins found that rising and chronic inflammation in middle and late age are linked to brain change in people with poor cognition and dementia.
The authors suggest that efforts to curb inflammation with drugs or lifestyle changes midlife or earlier may be key to delaying or preventing cognitive decline in old age.
The study analyzed data gathered from a federally funded study on more than 1,500 people.
Previous research has shown that chronic inflammation and the biochemicals associated with it may damage the brain.
C-reactive protein, an inflammatory factor made in the liver, for example, already has become a marker for chemical damage to heart and blood vessel tissue indicative of heart attack.
So far, however, studies linking inflammation to brain abnormalities have not looked at these factors over an extended period of time in the same population.
In the new study, the team took data from the atherosclerosis risk in communities (ARIC) study.
The study looked at brain structure and integrity, as well as a marker of inflammation over a 21-year period spanning middle age to late life.
They focused on and compared data on 1,532 participants recruited from 1987 to 1989 from Washington County, Maryland; Forsyth County, North Carolina; Minneapolis, Minnesota; and Jackson, Mississippi.
Sixty-one percent of the participants were women, and 28% were African-American. At the final visit, participants were an average age of 76.
Over the course of the ARIC study, each participant had five visits with study coordinators, averaging every three years.
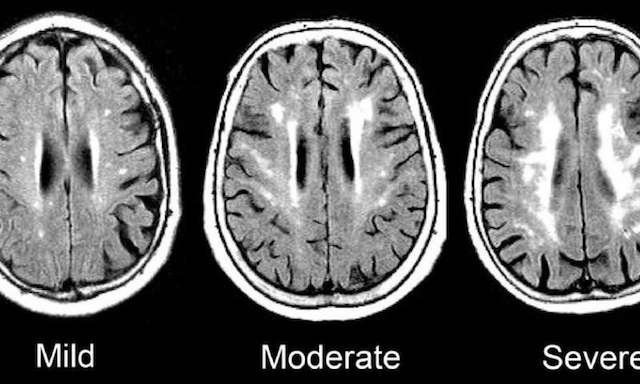
At the last visit, each participant underwent an MRI of their brain to examine evidence of damage to so-called white matter—the part of the brain responsible for transmitting messages.
The damaged white matter appears superwhite on a scan, similar to overexposure on a photograph, and was measured using an automated program.
At visits 2, 4 and 5, the researchers took blood samples to measure for high-sensitivity C-reactive protein, a standard measure of inflammation throughout the body.
Those with levels below 3 milligrams per liter were considered to have low inflammation, whereas those with 3 or more milligrams per liter of C-reactive protein were considered to have elevated inflammation.
The researchers found that the 90 people who transitioned from low to persistently elevated C-reactive protein during midlife showed increasing inflammation and the greatest damage to the white matter in the brain.
The team says their findings overall showed that increasing and chronic inflammation were associated with the most damage to white matter.
There is more reason to infer a cause and effect relationship between growing and persistent inflammation and evidence of dementia.
More studies would need to be done to prove cause and effect and figure out the precise pathways to brain damage.
Common causes of chronic inflammation include cardiovascular disease, heart failure, diabetes, high blood pressure and infections such as hepatitis C or HIV.
Inflammation is a normal byproduct of aging, but poor physical health and injuries seem to exacerbate it.
Some studies suggest that reducing inflammation in the short term can be accomplished by treating and controlling common cardiovascular diseases and maintaining a healthy weight.
The study is published in the Neurobiology of Aging.
Copyright © 2018 Knowridge Science Report. All rights reserved.



